
What Causes Chronic Lower Back Pain? (And What Actually Helps Fix It)
You wake up, and before your feet even hit the floor, there it is, that deep, dull ache in your lower back. You try to stretch it out. Roll over carefully. Maybe tell yourself it’ll loosen up once you start moving. Sometimes it does. Most days? It just… stays. Like background noise you can’t turn off.
If that sounds like your morning, you’re not alone. Not even a little bit.
We see this every single week at Surge Wellness here in Surrey, BC. People in their 30s, 40s, and 50s; teachers; warehouse workers; software developers; and parents who've been dealing with chronic lower back pain for months, sometimes years. They’ve tried the YouTube stretches. Bought the Amazon lumbar pillow. I took ibuprofen until the bottle ran out. And nothing really stuck.
The worst part? A lot of them have been told to just “rest more” or that it’s “just part of getting older.” So they accept it. They stop expecting to feel better. They rearrange their whole life around the pain without even realizing they’re doing it.
That’s not okay. And honestly, it doesn’t have to be that way.
Here’s the bigger picture. Back pain affects around 80% of adults at some point during their lifetime. In Canada, the government’s own Pain Task Force projected that over 8 million Canadians would be living with chronic pain by 2025, and the lower back is far and away the most common site. It ranks as the top reason people under 60 see a doctor in this country. Worldwide, it’s the leading cause of years lived with disability.
Those numbers are staggering. But what I find more concerning is how many people just… put up with it. They Googled their symptoms at 2 a.m. They try random fixes. They push through. And the pain slowly takes over more and more of their daily life without them even realizing it.
I wrote this post because I wanted to put something genuinely useful out there. Not a generic “10 tips for back pain” listicle. Not a sales pitch disguised as health advice. Just a real, detailed breakdown of what causes chronic lower back pain, why it sticks around, and what actually works to fix it, based on what we see every day clinically and what the research supports.
Fair warning: it’s a long read. Grab a coffee. Your back will thank you.

So What Actually Counts as “Chronic” Back Pain?
People use the word “chronic” pretty loosely, so let me clarify.
Clinically, back pain falls into three categories. There’s acute pain; that’s the fresh stuff, usually from a specific incident. Lifted something too heavy, tweaked your back in the gym, slept in a weird position. It’s been there less than four weeks. Then you’ve got sub-acute, which hangs around between four and twelve weeks. And then there’s chronic: anything past the twelve-week mark.
But here’s the thing most people don’t realize, and honestly, I wish more doctors explained this better. Just because your pain has stuck around for months doesn’t necessarily mean you’re still “injured” in the way you think. A lot of chronic lower back pain isn’t really about active tissue damage anymore. It’s about your nervous system staying on high alert. Your muscles have been compensating in weird ways for weeks and months. Your daily habits are feeding the cycle over and over.
That distinction really matters. Because it changes the entire approach to treatment. It’s one of the very first things our physiotherapists and RMTs assess when someone walks through the door at Surge.
The 7 Most Common Causes of Chronic Lower Back Pain
In most cases, there’s not one single thing you can point to and say, "That's it.” It’s usually several factors stacking up over time. Let me walk through the ones we see most often.
1. Sitting All Day (Yes, It Really Is That Bad)
I know you’ve heard this before. I know. But I’m going to say it anyway because the sheer number of patients we see whose back pain traces directly to their desk setup is kind of unbelievable.
If you’re working a desk job, and in Surrey’s growing tech and admin sectors, a lot of you are, you’re probably spending 7 to 10 hours a day in a seated position. Over weeks, months, and years, that compresses your lumbar spine, tightens your hip flexors into angry little knots, and turns your glutes and core muscles into something resembling decorative accessories.
Your body is adaptable. Incredibly so. But it adapts to whatever you do most. And if what you do most is sit hunched over a laptop, your body literally reshapes itself around that posture. Then one day you bend down to pick up your kid’s backpack and, bam. Something “goes.” But really, it’s been going for a while.
2. Muscle Imbalances and Weak Core Stability
Your lower back was never meant to handle everything on its own. It relies on a whole team: your abdominals, your glutes, your pelvic floor, and the deep stabilizer muscles running along your spine. When everything’s working together, the load is shared, and your spine is happy.
The problem is, most people have at least a couple of weak links in that chain. Glutes that have basically forgotten how to fire because you sit on them all day. Core muscles that haven’t been properly engaged since… well, ever. Tight hip flexors pulling everything forward.
So your lower back compensates. It picks up the slack. And it does that admirably for a while, until it doesn’t. And then you’re on our table.
3. Disc Issues, Bulging and Herniated Discs
The discs between your vertebrae act as shock absorbers. Over time, or after a specific injury, the tough outer layer of a disc can weaken, and the softer inner material pushes out. If it presses on a nerve, you’ll know about it, radiating pain down the leg, numbness, tingling, and sometimes weakness.
I know disc problems sound terrifying. But here’s what I want you to hear: many disc bulges are manageable without surgery. I’ll say that again. Many disc bulges are manageable without surgery. The right combination of physiotherapy and hands-on treatment can make a huge difference. Surgery is a last resort, not a first answer, and any good practitioner will tell you that.
4. Degenerative Changes (Osteoarthritis, Spinal Stenosis)
As we get older, the joints and discs in the spine gradually wear down. That’s just biology. Osteoarthritis in the lumbar spine is extremely common in people over 40, and spinal stenosis, where the spinal canal narrows, shows up more frequently with age too.
But here’s something that might surprise you. Degenerative changes on an MRI don’t always mean you’ll be in pain. Seriously. There are loads of people walking around with “worn” discs and arthritic joints who feel perfectly fine. The pain tends to show up when there’s also inflammation, muscle tension, or movement dysfunction layered on top.
I bring this up because a lot of people get an MRI, see the word “degeneration,” and panic. Don’t. Context matters way more than imaging alone.
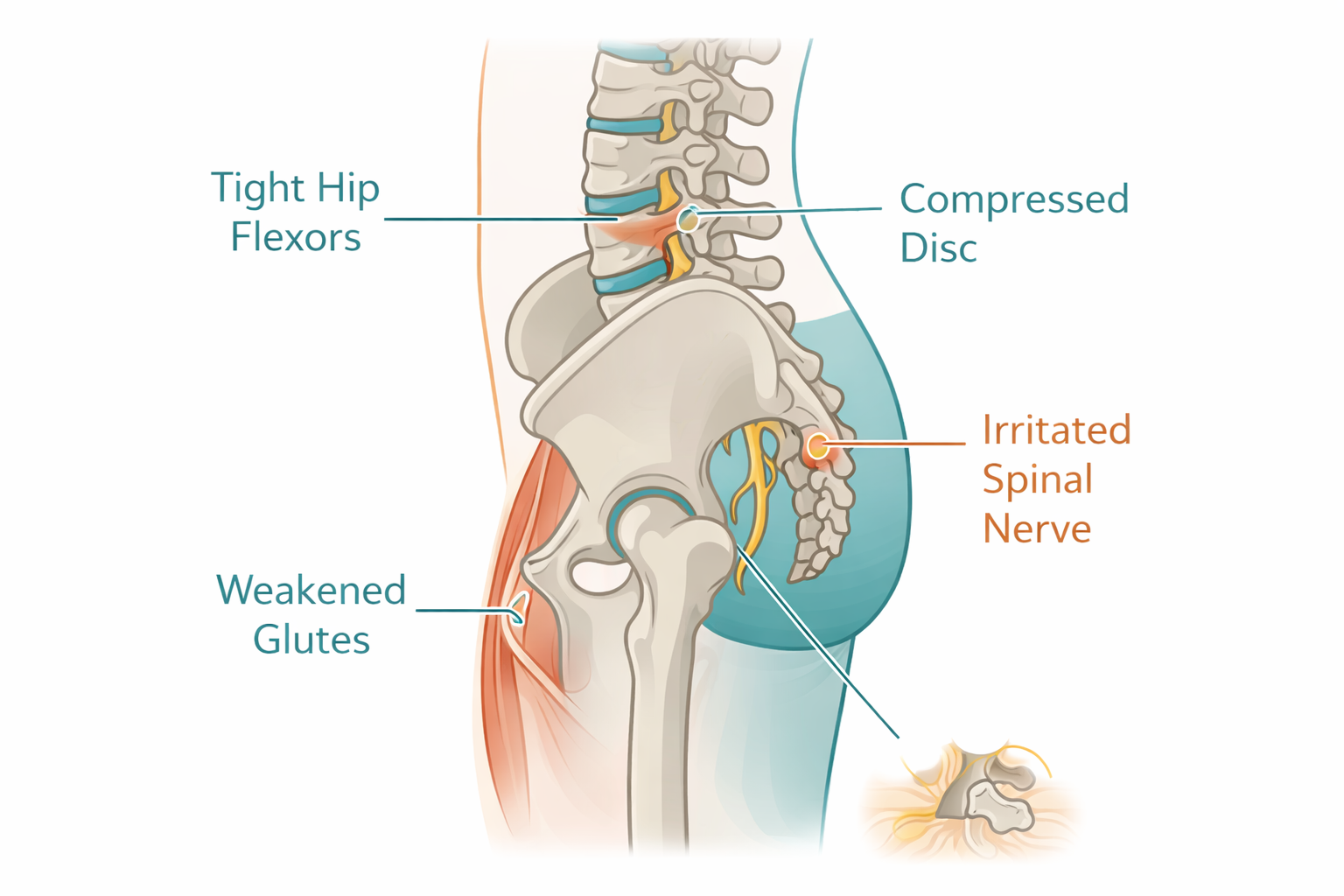
5. Sciatica and Nerve Irritation
If your back pain shoots down one leg, sometimes all the way to your foot, there’s a good chance the sciatic nerve is involved. Sciatica isn’t a diagnosis in itself, really. It’s a symptom. Usually caused by a disc herniation, bone spur, or a tight piriformis muscle squeezing the nerve.
The encouraging part: most sciatica responds well to conservative treatment. Physio to take the pressure off the nerve, massage therapy to release the surrounding muscle tension, that combination can make a noticeable difference in a matter of weeks. We’ve had patients who came in barely able to sit down drive home after six sessions saying they felt like a different person. (Not every case, of course. But often enough that I feel confident saying it.)
6. Stress. Seriously.
This one catches people off guard, but it really shouldn’t. We have strong evidence now that psychological stress, anxiety, and unresolved emotional tension can directly amplify chronic pain, particularly in the lower back.
When you’re stressed, your body braces. Your muscles tighten. Your nervous system stays in this heightened, almost fight-or-flight state, which turns up the volume on pain signals. It’s not that the pain is “all in your head.” I hate that phrase, honestly. Your head and your body aren’t separate systems. They’re deeply, physically wired together.
This is one reason we try to take a whole-person approach at Surge Wellness. If we just treat the muscles without paying attention to stress, sleep, and overall wellbeing, we’re basically mopping the floor with the tap still running.
7. Old Injuries and Motor Vehicle Accidents
A huge chunk of the chronic back pain we treat in Surrey started with a specific event, a car accident, a sports injury, a bad fall. The initial injury may have healed in the traditional sense, but the body often holds onto compensatory movement patterns. You start moving differently to protect the area that was hurt, and over time, those new patterns create their own set of problems.
This is incredibly common with ICBC claims. Someone gets rear-ended. They do a few weeks of treatment, start feeling “good enough,” and stop. Then six months later, the pain creeps back, different spot, different quality, but still connected to that original accident. I wish more people understood how important follow-through is in these cases.
When Should You Actually Go See Someone?
Okay, real talk. The honest answer is: probably sooner than you’re planning to.
I get it. There’s this cultural thing where we feel like we should tough it out. Try some stretches from Instagram. Wait and see. And for a minor muscle tweak, sure, that’s often fine. But if any of the following sound familiar, it’s time to get it properly looked at:
•Your pain has hung around for more than 2 to 3 weeks without real improvement
•It radiates down your leg, or you’re getting numbness or tingling
•You’re losing range of motion, can’t bend, twist, or stand up straight without wincing
•The pain is waking you up at night
•You were in a car accident or had a significant injury
•Everyday stuff, sitting at your desk, driving, picking up your kids, is getting harder
•Over-the-counter painkillers aren’t really doing anything anymore
None of those are signs of weakness. They’re your body telling you it needs help. And I’ll be blunt here: the people who come in early almost always do better than the ones who white-knuckle it for months. We see this constantly. The early birds bounce back in weeks. The people who waited a year? They still improve, but it takes significantly longer and the road is harder.
If someone has told you to “just rest” for chronic back pain, please know that is outdated advice. Prolonged rest for chronic pain actually makes things worse in most cases. The research on this is very clear. Movement, the right kind, guided by a professional, is medicine.

What Massage Therapy Actually Does for Chronic Lower Back Pain
This is where I get a bit passionate, so bear with me.
Registered Massage Therapy, RMT, is one of the most studied hands-on treatments for chronic lower back pain. And I don’t mean “studied” in a loose, wellness-blog kind of way. I mean proper peer-reviewed research.
A Cochrane systematic review (basically the gold standard for medical evidence) found that massage therapy produced meaningful improvements in both pain and function for people with sub-acute and chronic lower back pain. A separate study published in the Annals of Internal Medicine found that patients receiving weekly massage sessions saw clinically significant improvements compared to usual care alone, improvements that held up at six months post-treatment.
And then there’s a real-world study published in Pain Medicine that I find particularly compelling. Instead of a controlled lab environment, they studied massage as it actually happens, patients referred by a doctor, treated in a real clinic, getting a series of 10 sessions. Over half the participants experienced what the researchers classified as clinically meaningful improvement. Not just “felt a bit better.” Clinically meaningful.
So what exactly is happening when an RMT works on your back? Here’s the short version:
•They’re releasing tight, overworked muscles that are pulling your spine out of its natural alignment
•Increasing blood flow to inflamed or damaged tissues, which genuinely speeds up healing
•Activating your body’s natural pain-relief pathways (your nervous system has built-in volume dials, basically)
•Breaking up adhesions and scar tissue that are limiting how you move
•Bringing down cortisol levels, which directly reduces that stress-driven muscle tension we talked about earlier
I want to be clear about something, though. At Surge Wellness, our RMTs aren’t doing generic spa-style relaxation rubs for people with chronic back pain. (Unless that’s what you want and need, which is totally valid too.) For chronic pain, they use targeted approaches, deep tissue work, myofascial release, trigger point therapy, based on a proper assessment of what’s going on with your specific body.
To give you a real example, we had a patient a few months ago, a desk worker in her late 30s, who came in with pain she’d been carrying for over a year. After her initial assessment, she started with twice-weekly RMT sessions focused on her hip flexors, QL muscles, and thoracolumbar fascia. Within three weeks, her daily pain had dropped from what she described as a “constant 6 out of 10” to a “maybe 3 on a bad day.” That’s when we started layering in physio. Stories like that aren’t rare here. They’re kind of our whole thing.
How Physiotherapy Gets to the Root Cause
If massage is about relieving the tension and calming things down, physiotherapy is about figuring out why the pain keeps showing up, and fixing that.
Our physios start with a pretty thorough assessment. They watch how you move. They test which muscles are firing properly and which ones are basically asleep. They look at your posture, your joint mobility, your movement patterns, things you probably don’t even notice about yourself. And then they build a plan around what they actually find, not around a generic template.
For chronic lower back pain, a physio plan typically includes some combination of:
•Manual therapy, hands-on joint mobilizations and soft tissue work
•Targeted therapeutic exercise, strengthening programs aimed at your specific weak links
•Postural correction, retraining how you sit, stand, and move day-to-day
•Education, and this one is underrated, honestly. Helping you understand your pain makes it feel less frightening and more manageable
•Modalities like IFC, ultrasound, or heat when appropriate for short-term pain relief
The evidence base here is solid. Active, exercise-based physiotherapy is consistently shown to be one of the most effective long-term treatments for chronic lower back pain. It doesn’t just bring the pain down. It reduces the odds of it coming back. Which, when you think about it, is really what everyone wants.
And for anyone here in Surrey dealing with an ICBC claim, physiotherapy is typically covered. Our team handles the paperwork and billing, so you’re not adding admin stress to an already stressful situation.
RMT or Physiotherapy, Do You Need One or Both?
This might be the question we get asked more than any other. And my honest answer, for most people with chronic back pain, is: both. But let me explain why.
Massage therapy is fantastic at bringing down your immediate pain levels, releasing tension that’s built up over weeks or months, and calming an overactive nervous system. It gives you relief. Physiotherapy is more of the long game, building strength, correcting how you move, addressing the underlying reasons the pain developed in the first place.
They’re not competing treatments. They actually work better together.
What we often see at Surge is this: a patient starts with a few RMT sessions to get their pain to a manageable level. Then we layer in physiotherapy to start tackling the root causes. Over time, the massage sessions taper off, maybe once every few weeks for maintenance, while the physio exercises become part of their daily routine at home.
That combination, honestly, is where the magic happens. I’ve seen it work too many times to count.
Not sure where to start? That’s fine. Book an initial assessment and we’ll sort it out together. No pressure, no upsell. Just a conversation about what’s going on and what makes sense for you.

5 Things You Can Start Doing Today (Seriously, Today)
While you figure out your treatment plan, here are a handful of things that can genuinely help. They’re not magic. But they’re real, and they add up.
1. Get Up and Move Every 30 to 45 Minutes
Set a timer on your phone if you have to. Walk around your office. Do some gentle stretches by your desk. The single worst thing for a chronic lower back is staying stuck in one position for hours on end. Your spine craves movement. Give it some.
2. Actually Strengthen Your Core (Not Crunches)
When I say core work, I’m not talking about doing 200 crunches. Crunches can actually make lower back pain worse, look it up. I’m talking about planks, bird-dogs, dead bugs, glute bridges. Exercises that build stability around your spine without loading it further. If you’re not sure where to start, a physiotherapist can set you up with a routine in one session.
3. Stretch Those Hip Flexors
Tight hip flexors are probably the sneakiest contributor to lower back pain that nobody talks about enough. A simple kneeling hip flexor stretch, 30 seconds on each side, twice a day. That’s it. Do it for two weeks and tell me you don’t notice a difference. I’ll wait.
4. Change How You Sleep
Stomach sleepers, I’m sorry, but your lower back hates you for it. Try sleeping on your side with a pillow between your knees, or on your back with a pillow tucked under your knees. It keeps your spine in a more neutral position overnight. Small change, surprisingly big impact.
5. Do Something About Your Stress
Yeah, yeah. Easier said than done. I hear you. But even small things count, a 10-minute walk outside at lunch, some slow deep breathing before bed, putting your phone down an hour before you sleep. Stress and back pain feed each other in a vicious loop. You don’t have to meditate on a mountaintop. Just do one small thing differently.

Why Going Local in Surrey Actually Matters
I’m biased here, obviously. But let me make the case anyway.
Chronic back pain doesn’t get fixed in one visit. It takes regular, consistent care over weeks and sometimes months. And consistency becomes a whole lot easier when your clinic is ten minutes from your house or your office, not a 45-minute slog across the city through Surrey traffic.
At Surge Wellness, our patients pop in for a lunch-hour physio session, or they book a massage right after work. They don’t have to plan half their day around getting treatment. That matters way more than people think. Because honestly? The best treatment plan in the world is useless if the logistics make it impossible to actually show up.
We also know this community. We understand the desk-heavy work cultures, the commuter lifestyles, the ICBC claims from Highway 1 fender-benders. That local context shapes how we approach care, and our patients appreciate it.
Speaking of which, we handle ICBC claims, extended health benefits, and direct billing. So you’re not drowning in paperwork when you should be focused on feeling better.
Frequently Asked Questions
How long does it take for chronic lower back pain to actually improve?
It depends. Some people feel a real shift in 4 to 6 weeks of consistent treatment. More complex or long-standing cases can take 3 to 6 months. There’s no honest one-size-fits-all answer. But the key is treating the root cause, not just masking symptoms with painkillers. The sooner you start, the shorter the road tends to be.
Is massage therapy covered by ICBC in British Columbia?
Yes, if your back pain is connected to a motor vehicle accident, RMT and physiotherapy can both be covered under your ICBC claim. Our team at Surge Wellness can walk you through the referral and billing process, we do it all the time.
Can I see both an RMT and a physiotherapist at the same clinic?
Absolutely. That’s actually one of the biggest advantages of a multidisciplinary clinic like ours. When your RMT and physio are under the same roof, they can communicate about your progress and coordinate your care. It’s a much more seamless experience than bouncing between separate practices.
Do I need an MRI for my lower back pain?
Probably not right away. Most lower back pain can be accurately assessed through a hands-on physical examination. Imaging is usually only recommended when there are red flags, significant weakness, bowel or bladder changes, or pain that isn’t responding to treatment at all. Your physiotherapist will let you know if imaging is warranted.
What’s the difference between a massage therapist and an RMT?
In British Columbia, a Registered Massage Therapist (RMT) is a regulated healthcare professional. They’ve completed rigorous education, passed provincial licensing exams, and are held to professional clinical standards. Their treatments are eligible for extended health insurance coverage. A general “massage therapist” without RMT credentials may not have the same level of training or accountability. When it comes to treating chronic pain, that distinction matters.
How often should I get massage therapy for chronic back pain?
During the initial treatment phase, once or twice a week is typical. As your pain goes down and your function improves, we usually taper to every two weeks, then monthly for maintenance. Your RMT will recommend a schedule based on how your body responds, there’s no rigid formula.
Is lower back pain just a normal part of aging?
Common? Sure. Normal? No. Age-related changes in the spine h
appen to everyone. But pain and disability are not inevitable. The right mix of exercise, manual therapy, and lifestyle adjustments can keep you active and comfortable well into your later years. I’ve treated patients in their 70s who move better than some 35-year-olds. It’s about what you do, not just how old you are.
Ready to Get Your Back Feeling Like Itself Again?
If you’ve read this far, your back pain probably isn’t minor. It’s affecting your work, your sleep, your mood, your ability to do the things you actually enjoy. And that’s exactly why we’re here.
At Surge Wellness in Surrey, BC, we combine registered massage therapy and physiotherapy to treat chronic lower back pain from every angle. We’ll figure out what’s actually going on, build a plan that fits your life, and walk through it with you step by step.
No judgment. No sales pitch. Just good care from people who actually care.
→ Book Your Appointment at Surge Wellness Today
Call us, book online, or just walk in. We’re here.



