
Sciatica Pain That Won’t Go Away? Here’s What’s Really Going On (And What to Do About It)
There’s a particular kind of pain that makes people stop mid-sentence. It shoots from your lower back, down through your glute, and races down the back of your leg like an electrical current. Sometimes it reaches your calf. Sometimes it goes all the way to your foot. And sometimes it comes out of absolutely nowhere while you’re doing something as mundane as picking up a sock off the floor.
That’s sciatica. And if you’re reading this, there’s a decent chance you already know exactly what I’m talking about.
Sciatica is one of the most common reasons people come to see us at Surge Wellness here in Surrey, BC. And the frustration level is usually pretty high by the time they walk through the door. They’ve been dealing with it for weeks, sometimes months. They’ve tried stretching, heat packs, and anti-inflammatories. Some have even been told it’ll "just go away on its own." And sometimes it does. But when it doesn’t? That’s when things start to get really disruptive.
So let’s talk about what sciatica actually is, what’s causing yours, and what treatments genuinely work. Not the watered-down advice you get from a five-minute Google search. The real stuff.

What Is Sciatica, Exactly?
First, let’s clear up a common misconception. Sciatica is not a diagnosis. It’s a symptom. It describes a pattern of pain that radiates along the path of the sciatic nerve, which runs from your lower spine, through your buttock, and down each leg.
When people say "I have sciatica," what they really mean is "something is irritating my sciatic nerve, and it’s causing pain down my leg." The important question is: what’s doing the irritating?
The sciatic nerve is the longest and thickest nerve in your body. It’s made up of five nerve roots that exit from the lower lumbar and upper sacral spine. When any of those roots get compressed, inflamed, or irritated, you feel it. And because the nerve runs so far, the pain can show up pretty much anywhere along that path.
That’s why some people feel it in their glute, some feel it behind their knee, and some feel tingling in their toes. Same nerve, different location of irritation.
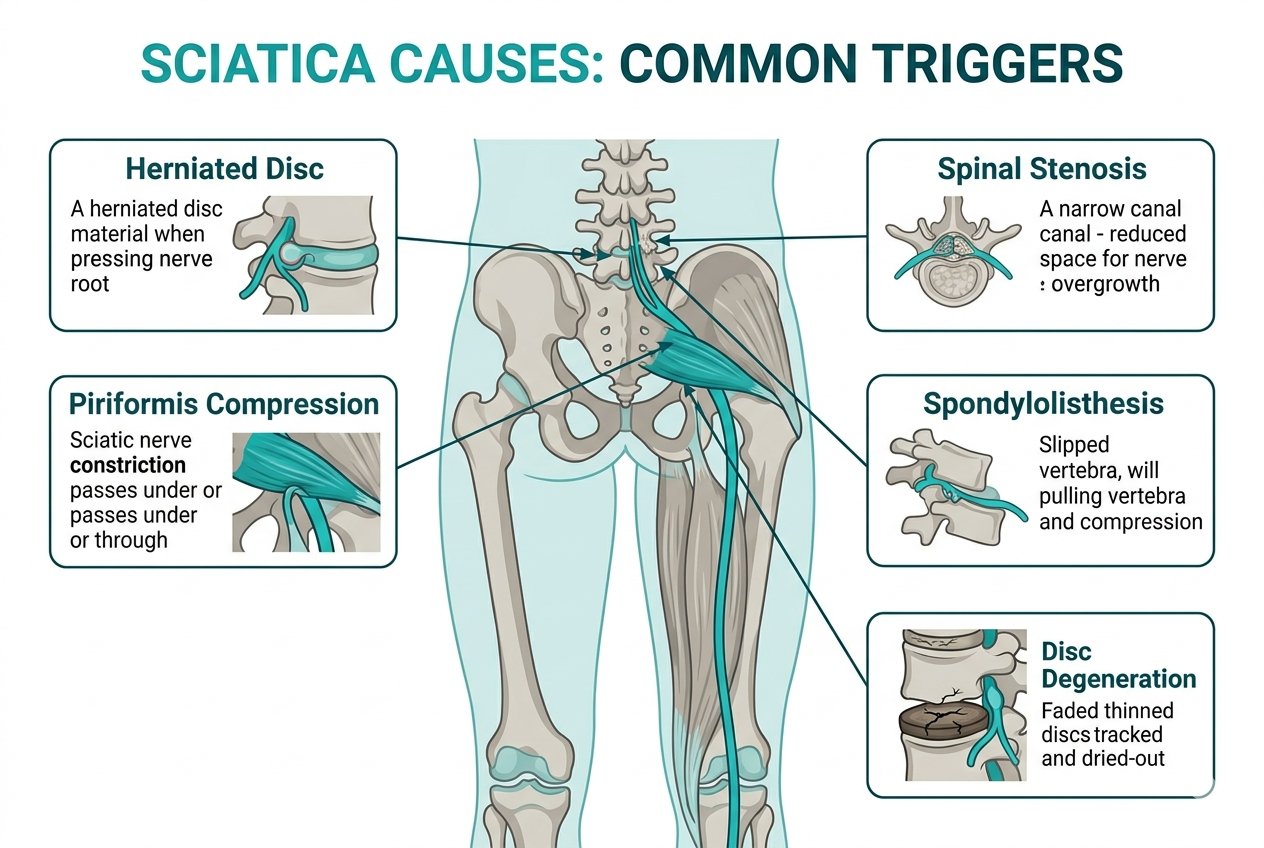
The 5 Most Common Causes of Sciatica (And Which One You Probably Have)
This is where it gets useful. Because understanding the cause changes the treatment. And at Surge Wellness, identifying the root cause is always step one.
1. Herniated or Bulging Disc
This is the most frequent culprit. A disc in your lower spine pushes outward and presses against one of the nerve roots that form the sciatic nerve. It’s especially common at the L4-L5 and L5-S1 levels. If your sciatica came on suddenly after bending, lifting, or twisting, a disc issue is likely the reason.
The good news? Most disc herniations that cause sciatica respond well to conservative treatment. The body can actually reabsorb the herniated material over time, especially when you’re doing the right exercises and getting proper hands-on care. Surgery is rarely necessary.
2. Piriformis Syndrome
This one flies under the radar a lot. The piriformis is a small muscle deep in your buttocks. In some people, the sciatic nerve runs right through it. When the piriformis gets tight or goes into spasm, it squeezes the nerve and mimics all the symptoms of a disc-related sciatica.
Here’s how to tell the difference: piriformis syndrome tends to produce pain that’s centred more in the glute than the lower back. It usually gets worse with sitting (especially on hard surfaces) and during activities like climbing stairs or crossing your legs.
This is one of the conditions that responds beautifully to registered massage therapy. An RMT who knows what they’re doing can release the piriformis and take the pressure off the nerve, often within a few sessions.
3. Spinal Stenosis
As we age, the spinal canal can narrow due to degenerative changes, bone spurs, or thickened ligaments. When that narrowing compresses the nerve roots, you get symptoms down the leg. This type of sciatica tends to develop gradually rather than suddenly, and it’s more common in people over 50.
People with stenosis-related sciatica often notice that their symptoms get worse when they stand or walk for long periods and improve when they sit or lean forward (like over a shopping cart). That positional pattern is a strong clue.
4. Degenerative Disc Disease
Despite the scary-sounding name, this is really just the natural ageing process of your spinal discs. Over time, discs lose hydration and height, which can narrow the spaces where the nerve roots exit the spine. If the narrowing is significant enough, it can irritate the sciatic nerve.
Degenerative changes are nearly universal in people over 40 on imaging, but they don’t always cause symptoms. The pain usually shows up when there’s a combination of disc degeneration, inflammation, and muscle dysfunction all happening together.
5. Spondylolisthesis
This is when one vertebra slips slightly forward over the one below it. If the slip is enough to narrow the nerve canal or put pressure on a nerve root, sciatica can develop. It’s most common in the lower lumbar spine and can be caused by a stress fracture, degenerative changes, or, less commonly, a traumatic injury.
Most cases of spondylolisthesis are mild and manageable with physiotherapy focused on core stability and spinal alignment.
How Do You Know If It’s Actually Sciatica?
Not all leg pain is sciatica. That’s important. Hip bursitis, hamstring strains, and referred pain from the lower back can all mimic sciatica without involving the sciatic nerve at all. And the treatment for each of those is different.
True sciatica typically has a few hallmark features:
Pain that starts in the lower back or buttocks and radiates down one leg (rarely both)
The pain follows a specific path, usually down the back or outside of the leg
You may feel numbness, tingling, or a pins-and-needles sensation along that path
There might be weakness in the affected leg, like difficulty lifting your foot (foot drop)
Sitting, coughing, or sneezing can make it worse
The pain is often described as burning, sharp, or electric rather than a dull ache
If you’re experiencing these symptoms, it’s worth getting a proper assessment. At Surge Wellness, our physiotherapists use specific clinical tests (like the straight leg raise test and neurological screening) to determine whether the sciatic nerve is truly involved and, if so, where the compression is coming from. That assessment is the foundation of everything else.
When Sciatica Needs Professional Attention (Don’t Wait on These)
Mild sciatica can sometimes resolve on its own within a few weeks. But if any of the following apply, you should get it looked at sooner rather than later:
The pain has lasted more than 3 to 4 weeks without improvement
You’re experiencing progressive numbness or weakness in your leg or foot
The pain is severe enough to interfere with sleep, work, or daily activities
You have difficulty controlling your bladder or bowel (this is rare but requires immediate medical attention)
The pain started after a car accident or significant injury
I want to be very direct about this: the "wait and see" approach works for mild cases, but it’s a terrible strategy for sciatica that’s getting worse. Nerve irritation that persists for months can lead to sensitisation, where the nerve becomes increasingly reactive and harder to calm down. The earlier you intervene, the shorter and smoother the recovery.
How Massage Therapy Treats Sciatica
This is where I get to champion something I’ve seen work over and over again.
A lot of people don’t realise that massage therapy can be one of the most effective treatments for sciatica, especially when the cause is muscular (like piriformis syndrome) or when tight muscles around the spine are contributing to nerve compression.
When you have sciatica, the muscles in your lower back, glutes, and hips don’t just sit there passively. They react. They tighten up, they guard, they spasm. And that reactive muscle tension often makes the nerve compression worse. It’s a vicious cycle: the nerve irritation causes muscle guarding, and the muscle guarding increases the pressure on the nerve.
An experienced RMT breaks that cycle. Here’s what treatment typically involves for sciatica:
Deep tissue release of the piriformis and deep external rotators of the hip, taking direct pressure off the sciatic nerve
Myofascial release along the lumbar paraspinals and quadratus lumborum to reduce spinal compression
Trigger point therapy in the glutes, where referred pain patterns often overlap with the sciatic nerve distribution
Gentle hamstring and hip flexor work to restore length and reduce the pulling forces on the pelvis and lower spine
Nervous system calming techniques, because when you’ve been in pain for weeks, your fight-or-flight response is often stuck in overdrive
We had a patient last spring, a personal trainer in her early 30s, who had been dealing with piriformis-related sciatica for about four months. She’d been stretching religiously, foam rolling daily, and it wasn’t getting better. After five targeted RMT sessions focused on her deep hip rotators and lumbar fascia, combined with a few specific exercises from our physio team, she was back to full training within six weeks. Her comment was something like, "I can’t believe I spent four months foam rolling when I needed someone to actually get in there." She wasn’t wrong.
If you’ve already read our earlier article on massage for sciatica, you’ll know we’re big believers in this approach. This post goes deeper on the clinical side.
How Physiotherapy Fixes the Root Cause of Sciatica
Massage therapy is fantastic for relieving muscle tension and calming the nerves. But if you want the sciatica to stay gone, physiotherapy is what makes that happen.
A physiotherapist looking at sciatica will go beyond the symptom. They’ll assess your spinal mobility, your hip mechanics, your core strength, your movement patterns, and your posture to figure out why the nerve got compressed in the first place.
A physio plan for sciatica at Surge Wellness typically includes:
Directional preference exercises: specific movements (often extension-based for disc herniations) that help centralise the pain, meaning they pull the symptoms back up from the leg toward the spine. This is a very good sign in treatment
Nerve gliding and flossing: gentle, controlled movements that help the sciatic nerve slide freely through the surrounding tissues instead of getting stuck at a compression point
Core stabilisation: rebuilding the deep muscles (transversus abdominis, multifidus, pelvic floor) that protect the spine from further disc or joint issues
Hip mobility and strengthening: addressing weaknesses in the glutes and hip rotators that contribute to pelvic instability
Ergonomic and postural education: teaching you how to sit, lift, and move in ways that don’t aggravate the nerves
The nerve centralisation piece is worth highlighting. When your physiotherapist finds a movement that makes the leg pain retreat back toward the centre, that’s a very strong indicator that the disc or nerve is responding to treatment. Patients often notice this within the first few sessions. It’s one of the most satisfying things to see in a clinic.
For ICBC patients whose sciatica started after a car accident, physiotherapy is typically covered. We handle all the paperwork.
RMT Plus Physio: Why Both Together Work Best for Sciatica
You probably see where this is going. For sciatica, combining massage therapy and physiotherapy isn’t just a nice-to-have. It’s honestly the most effective approach we’ve found.
Massage releases the muscle compression around the nerve and gives you pain relief. Physio addresses the structural and movement issues that caused the compression. One without the other tends to leave part of the problem unsolved.
At Surge Wellness, your RMT and physiotherapist communicate about your case. If the RMT notices your piriformis keeps tightening up between sessions, they’ll flag it so the physio can look at why (often a weak gluteus medius). If the physio finds that a specific exercise is aggravating your symptoms, they’ll adjust and let the RMT know to focus on the reactive area.
That kind of coordination is hard to get when you’re seeing two different providers at two different clinics. Having everything under one roof matters.
How Long Does Sciatica Take to Heal?
I wish I could give you a clean answer. But the timeline depends on the cause and severity.
Piriformis Syndrome
Usually, the fastest to resolve. With consistent RMT and targeted exercises, most people see major improvement in 3 to 6 weeks. Full resolution in 6 to 10 weeks is typical.
Disc Herniation
More variable. Mild to moderate herniations with good treatment response can improve significantly in 6 to 12 weeks. More severe cases, or those with significant nerve compression, can take 3 to 6 months. The body’s ability to reabsorb herniated disc material is well documented in the research, but it takes time and the right rehab approach.
Spinal Stenosis
This is typically a management situation rather than a cure. Physiotherapy and massage can significantly reduce symptoms and improve function, but because the underlying narrowing is structural, ongoing maintenance is usually needed. The goal is to keep you active and comfortable, which is absolutely achievable.
Across all of these, the common thread is the same one I’ve repeated throughout every article we’ve published: early treatment shortens the timeline. Every time.
5 Things You Can Do at Home for Sciatica Relief
1. Try the McKenzie Press-Up
Lie face down and gently press your upper body up with your arms, keeping your hips on the ground. If this reduces or centralises your leg pain, it’s a very good sign, and you should keep doing it several times a day. If it makes the leg pain worse, stop and get assessed. The direction matters.
2. Don’t Sit for Long Stretches
Sitting compresses the lower lumbar discs and can increase pressure on the sciatic nerve. If you have to sit for work, get up every 20 to 30 minutes. Even a brief walk to the kitchen and back can take enough load off the nerves to keep symptoms manageable.
3. Walk, Don’t Run
Gentle walking is one of the best things you can do for sciatica. It promotes circulation, keeps the tissues mobile, and encourages the body’s natural healing processes. Running, however, puts a high-impact load through the spine. Stick to walking until your symptoms have settled.
4. Sleep on Your Side With a Pillow Between Your Knees
This keeps your pelvis neutral and reduces the stretch on the sciatic nerve overnight. If you’re a back sleeper, try placing a pillow under your knees instead. Stomach sleeping is the worst position for sciatica.
5. Stop Stretching Your Hamstrings (Seriously)
This one surprises people. When you have sciatica, your hamstrings might feel tight, but that tightness is often protective neural tension, not a muscle issue. Aggressively stretching the hamstrings can irritate the sciatic nerve further and make things worse. If you’re stretching your hamstrings and the pain increases, stop immediately. A physiotherapist can teach you nerve gliding techniques that are much safer.

Why Surge Wellness for Sciatica Treatment in Surrey
We’re local. We’re right here in Surrey, which matters when you need regular appointments and can’t afford to add a 45-minute commute to your already painful day.
We have both RMTs and physiotherapists under one roof, so your sciatica treatment is coordinated, not fragmented.
We direct bill ICBC and most extended health plans. No upfront costs for approved claims.
And we’ve treated a lot of sciatica. It’s one of the conditions we see most frequently, and our team knows how to identify the cause quickly and build a plan that actually works.
Frequently Asked Questions
Can sciatica go away on its own?
Mild sciatica sometimes resolves within a few weeks, especially if the cause is minor muscular tension. But moderate to severe sciatica, particularly from disc herniations or nerve compression, usually needs professional treatment to resolve fully. Waiting too long can allow nerve irritation to become chronic, making recovery longer and harder.
Is it safe to exercise with sciatica?
Yes, but the type of exercise matters a lot. Walking and specific therapeutic exercises (like nerve glides and extension-based movements) are usually helpful. High-impact activities, heavy lifting, and aggressive hamstring stretching can make things worse. A physiotherapist can give you a safe, individualised exercise plan.
Can massage make sciatica worse?
If done incorrectly, yes. Deep, aggressive massage directly over an acutely inflamed nerve can increase irritation. That’s why it’s important to see a registered massage therapist who understands sciatica and knows which muscles to target and which areas to avoid. At Surge Wellness, our RMTs are experienced with nerve-related conditions.
Do I need an MRI to diagnose sciatica?
In most cases, no. A thorough physical assessment by a physiotherapist can accurately identify the cause of sciatica without imaging. MRIs are typically recommended only if there are red flag symptoms (significant weakness, bladder changes), if the condition isn’t improving with treatment, or if surgery is being considered.
Is sciatica covered by ICBC?
If your sciatica developed after a motor vehicle accident, treatment is typically covered under your ICBC claim. Both RMT and physiotherapy are included. You don’t need a doctor’s referral to start, and we direct bill ICBC at Surge Wellness.
What’s the difference between sciatica and general low back pain?
General low back pain stays in the back. Sciatica involves radiating pain, numbness, or tingling that travels down the leg, following the path of the sciatic nerve. You can have both at the same time, but the treatment approach differs because nerve involvement requires specific techniques such as nerve gliding and directional preference exercises.
Ready to Get That Nerve Pain Sorted Out?
If sciatica is running your life right now, you don’t have to keep pushing through. At Surge Wellness in Surrey, BC, we’ll figure out exactly what’s causing your sciatic nerve pain and build a plan to fix it. RMT, physio, or both. Whatever your body needs.
→ Book Your Sciatica Assessment at Surge Wellness
Call us, book online, or walk in. Let’s get that nerve calmed down.



